Each year, between 300,000 and 700,000 individuals in the United States experience difficulty swallowing. This condition is referred to as dysphagia and commonly involves complications and pain or discomfort when swallowing, affecting a person’s ability to eat or drink.
While dysphagia can occur at any age, it is more common in older adults. This condition is experienced by 30% of adults more than 50 years of age, and up to 68% of nursing home residents. Dysphagia may be an acute or chronic condition.
People with dysphagia report having difficulty swallowing food or drinks, chewing, sucking, controlling saliva, taking medication, or protecting their airway from choking. If left untreated, ongoing problems can affect a person’s ability to meet their nutrition and hydration needs and can lead to mealtime anxieties due to choking risks or swallowing discomfort. Dysphagia may be an acute or chronic condition.
Common causes
The most common causes of dysphagia are related to underlying medical or physical conditions. Individuals may have impaired swallowing secondary to a variety of challenges including reduced mastication (chewing) or lost or missing teeth/dentures and reduced oral and pharyngeal sensitivity.
Dysphagia can often be caused by:
- Alzheimer’s disease
- Cerebral palsy
- Meningitis and brain tumors
- Mouth, throat, or esophageal cancer
- Multiple sclerosis
- Parkinson's disease
- Traumatic brain injury
- Spinal cord injury
- Stroke
Typically, a full assessment including a bedside swallowing evaluation, or a barium swallow study will be used to make a diagnosis.
Complications from dysphagia
A common warning sign of dysphagia is chronic coughing or choking while eating and gagging when swallowing. If a person does not receive treatment to help with their symptoms and continues to have challenges swallowing, especially when eating and drinking, they can be at risk for developing other health issues, including:
- Dehydration
- Malnutrition
- Pneumonia or respiratory infections
- Weight loss
- Anxiety and depression
Since dysphagia accompanies an underlying condition or is due to weakened or damaged muscles and nerves used for swallowing, diagnosing and treating what is causing the condition is essential to improving a person’s quality of life.
Treating dysphagia
Depending on the cause of the dysphagia, treatment may include swallowing exercises, positioning the head to allow for easier swallowing and prescribing medication to treat the condition causing the dysphagia.
Another effective way of managing dysphagia is modifying the texture of foods (chopped, minced, pureed) and thickening liquids to make eating and swallowing safer and easier. This helps reduce the risk of choking or having material enter the airway.
In the past, health care providers often used a variety of terms to describe diets for those requiring altered consistency foods, including “mechanical soft,” “blended smooth” and “chopped.” To help provide universal guidelines for the dysphagia diet, the International Dysphagia Diet Standardization Initiative (IDDSI) set out to standardize diets and liquid consistency. In 2019, the American Speech Language-Hearing Association and Academy of Nutrition and Dietetics endorsed the use of this International Dysphagia Diet.
Dysphagia diet
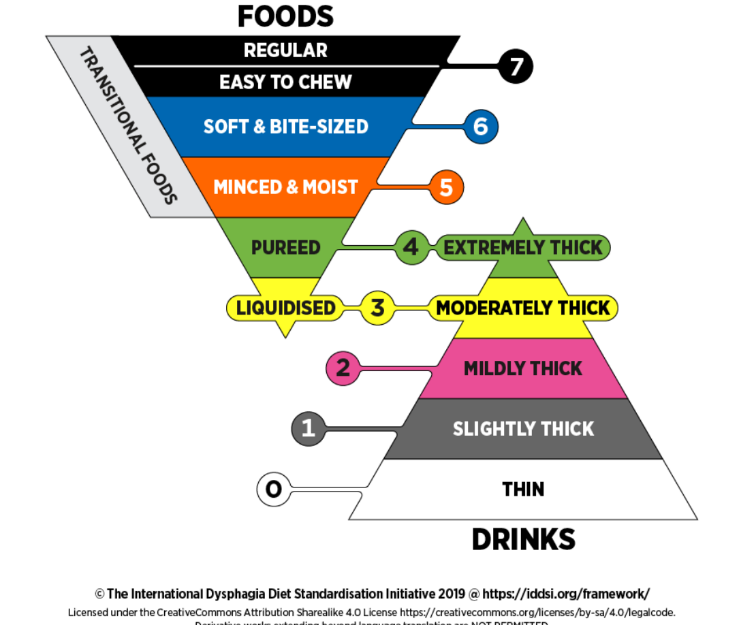
The IDDSI framework provides common terminology for describing food textures and drink thickness to improve safety for individuals with swallowing difficulties.
The IDDSI framework consists of a continuum of 8 levels (0 - 7). Drinks are categorized by their thickness and are assigned to a level between 0 and 4. Foods range from liquidized (level 3) to regular and easy to chew (level 7). This provides consistent terminology for providers to use to describe the precise level of texture modification needed for foods and thickness for drinks.
Mom’s Meals® can help
To accommodate the nutritional needs of individuals living with dysphagia, Mom’s Meals offers a pureed menu of fully prepared soft food meals. Our menu options have all been designed to meet the Academy of Nutrition and Dietetics requirement for Dysphagia (Level 1 - Pureed Nutritional Therapy).
While Mom’s Meals has not officially adopted the IDDSI guidelines, our pureed menu is intended to meet the guidelines of level 4 – pureed. Most of the meals would be considered level 6 or 7, soft and bite-sized or easy to chew. To meet level 5 – minced and moist criteria, the meals would need to be mashed or chopped up further and could be easily modified to this texture.

Brochure to share
Help others learn more about dysphagia and receive helpful tips in our brochure, Managing Your Dysphagia with Nutrition. Getting the proper nutrition can help people dealing with dysphagia live a healthier and more fulfilling life.