Humans have looked at food as medicine for centuries. Today, the growing body of evidence shows that it should be an integral part of everyone’s personal health plan. Health care stakeholders are taking note also.
In the nearly 2,500 years since humans first cultivated crops for medicinal purposes, the concept of “food as medicine” has remained an integral part of many Eastern healing practices. Today, the food as medicine movement is undergoing a renaissance of sorts — with growing recognition that what we eat plays an important role in disease prevention and management. This belief is buoyed by studies showing that even modest dietary adjustments can help to reverse the mortality rates attributable to food-related diseases, and that with certain diseases, long-term dietary changes can be as effective as pharmacological interventions — especially in the early stages.
While there is no single definition of the food as medicine concept, it is a recognition that diet has the potential to cause disease, as well as the ability to build, maintain and restore health. Regardless of what you call it — food as medicine, food is medicine, medically tailored meals, culinary medicine, food for health, prescription fruit and vegetable programs, culinary nutrition, or food for disease management — the concept is the same. It’s all about prioritizing food and diet to help prevent, reduce symptoms, or reverse a condition.
Dietary risk — a global issue
A study of health effects of dietary risks in 195 countries between 1990 and 2017 revealed that, in 2017, 11 million deaths were attributable to dietary factors — with high sodium intake, and low intake of fruit and whole grains among the primary culprits.
Pharmaceutical therapies used in combination with a medically tailored diet may be more effective than drugs alone. There are ample studies showing the health benefits of food as medicine and indicating that the emphasis should not be on diet or medicine alone, but rather on diet and medicine.
Focus on nutrition insecurity in the U.S.
According to the U.S. Department of Agriculture, over 47 million people are facing food insecurity in America. Chronic and diet-related conditions, including obesity, diabetes, cardiovascular disease, asthma, and stroke are among the leading causes of death in the U.S. — and disproportionately impact underserved and low-income communities.
The health of many such food-insecure populations has been improved by food as medicine programs and interventions designed not only to reduce food insecurity, but to also increase nutrition security with access to nutritious foods such as fruits and vegetables.
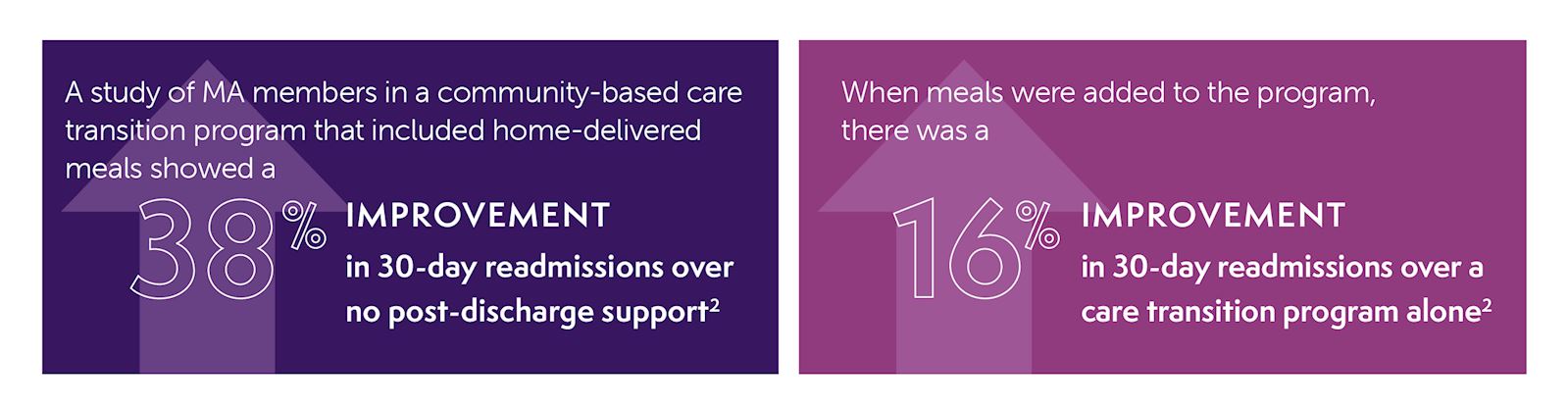
When someone is well-nourished, their risk of falling decreases, and their physical health improves. Research shows that people with chronic conditions who receive home-delivered meals experience fewer hospitalizations, and when hospitalized, their length of stay is significantly shorter.
Recognition and advocacy
Indeed, a growing number of health insurers, both public and private, are incorporating food as medicine into in their plans, and have initiated coverage for food interventions, including home-delivered meals, healthy grocery stipends and nutrition education. On the government side, policymakers and legislators are advocating food as medicine programs on local, state, and federal levels.
In addition, the Rockefeller Foundation committed $4.6 million in grants for equitable and community-directed approaches to scale food as medicine initiatives in the U.S. The funding will support organizations working to build partnerships with key stakeholders and bridge the gaps between food and health care. The goal is to help prevent, manage and treat diet-related illnesses among food-insecure Americans, and ensure more equitable access to foods that promote better health outcomes and reduce health costs.
Resource for you
The evidence in favor of food as medicine is clear, and now the commitments are being forged to increase awareness of the influence of nutrition on health, and to improve access to nutrient-rich foods for those who need it most. Ready to incorporate a medically tailored, home-delivered meal benefit into your plan? Mom’s Meals® can help.

Food as Medicine: What Health Care is Doing and What is Working
Our free white paper takes a deeper look at the food as medicine concept, chronic disease issues, and approaches from public and private sectors. You will also learn how our nutritious home-delivered meals can help improve health outcomes while advancing nutrition security.



.jpg)
