Lavinia Williams, a Californian who has congestive heart failure (CHF), teared up when she spoke of the pilot program facilitated by Mom’s Meals® and Inland Empire Health Plan: “If I wasn’t part of the program, I don’t think I would be here. They saved my life.”
Approximately 6.2 million American adults live with CHF, the ongoing inability of the heart to pump enough blood through the body to ensure a sufficient supply of oxygen.
Williams was one of 93 people with CHF who took part in an initiative that provided medically tailored meals and easy access to other health-related tools for a period of six months.
Many of the participants, including Williams, saw their medical condition improve and, in some cases, drastically.
Healthy foods help reduce hospitalizations
Launched in June 2021, the pilot program offered more than 28,000 fully prepared lower-sodium meals, fresh produce and dry goods; nutrition education; a digital scale; and home visits to select IEHP members in Riverside and San Bernardino counties in California. Each of the pilot participants had a minimum of two hospital stays within the previous year.
“The initiative clearly demonstrated that when individuals with this serious cardiac condition eat healthy foods over a period of time, it results in fewer hospitalizations and reduces the overall cost of care,” said Catherine Macpherson, MS, RDN., senior vice president of healthcare strategy and development, and chief nutrition officer for Mom’s Meals. “We hope to replicate these outstanding results in other similar populations.”
Dr. Gabriel Uribe, DSW, IEHP director of Community Health, said, “Patients with congestive heart failure tend to have a high rate of emergency room visits and hospitalizations. Upon discharge, they often lack social supports to effectuate successful lifestyle changes needed to improve chronic care. Our initiative showed that a holistic approach to managing the condition led to better patient outcomes, including fewer trips to the hospital.”
Pilot program results
During the first half of the program, Mom’s Meals provided three lower-sodium fully prepared meals per day. As the second half of the program approached, Mom’s Meals tapered fully prepared meals to two per day, then to one while also offering fresh produce and pantry boxes, delivered to the homes of pilot participants.
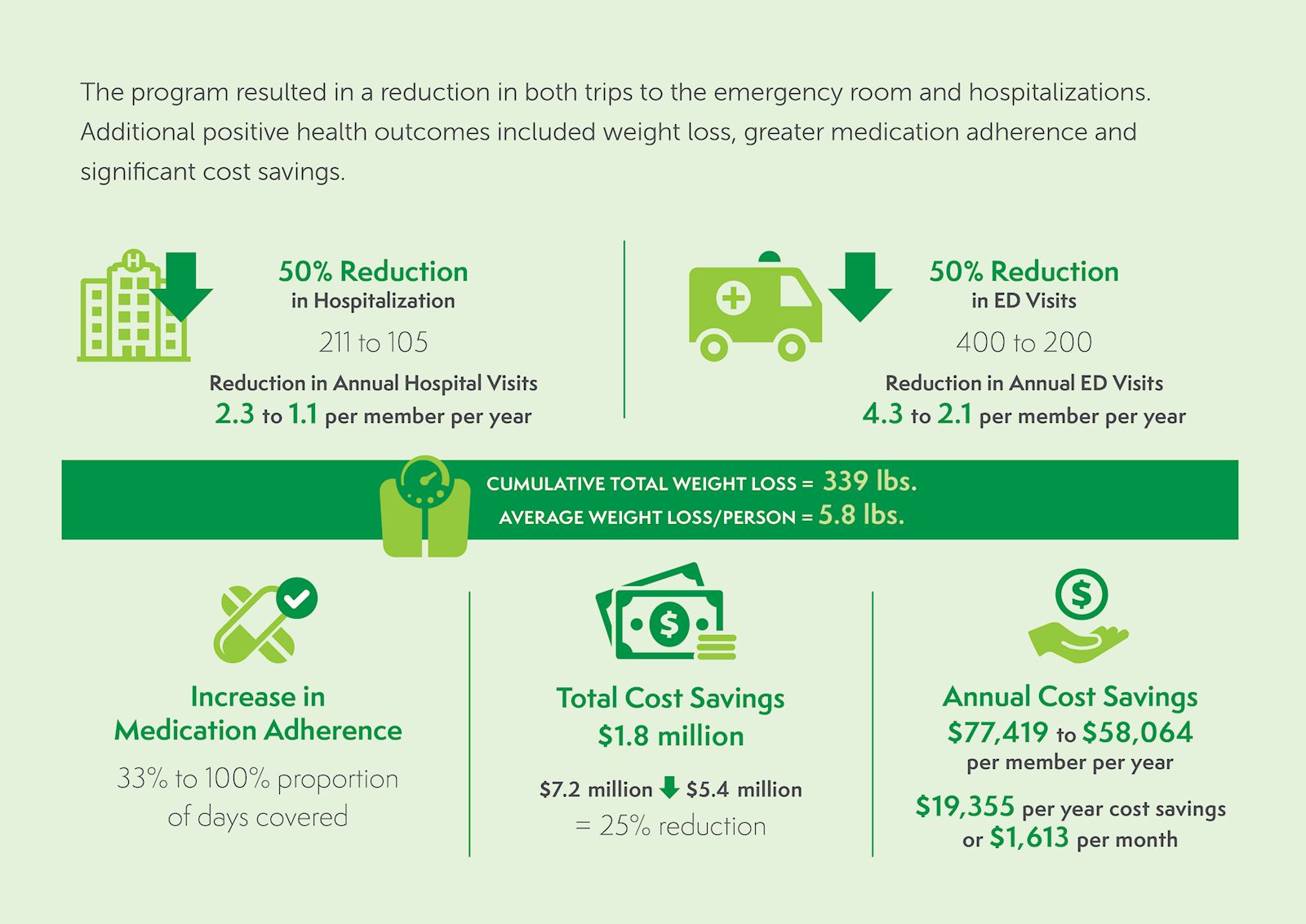
* This was primarily from decreased hospitalizations and associated costs.
Education and access to supplement nutrition
Along with nutrition education by Mom’s Meals’ registered dietitians and healthy recipes, members were supported in learning food preparation aligned with dietary guidelines for heart failure and received digital weight scales, delivered by IEHP’s “Health Navigators.” The scales allowed participants to track weight changes that might be due to fluid build-up in the body, which presents a risk for hospitalization. During home visits, Health Navigators also assisted participants in connecting to care management nurses, shared heart failure management plans, and conducted health risk assessments.
“One of our goals is to empower our members to be their healthiest selves,” Dr. Uribe added.
Reanalysis shows lasting impact
Data for 93 enrolled members was reanalyzed 6 months after first analysis; 12 months after program end date and found:
- 42% reduction in hospitalizations
- 39% reduction in length of stay
- 21% reduction in total cost of care
Members also self-reported:
- Improved access to healthy foods and lower salt consumption
- Reduced HF symptoms such as shortness of breath and swelling
Resources for you and your clients

For more insight, we have developed a suite of materials that includes a white paper, consumer brochure and articles that support the value of nutritious home-delivered meals to help improve heart health outcomes and costs. To learn more about how the Mom’s Meals team can help you support your clients, please contact us.



